A mystery illness was linked to Down syndrome. These moms found answers.
Before Sara Smythe began to disappear, she was thriving.
The youngest of four sisters, Sara was born with Down syndrome and lived the life of an active teen. At 13, the Toledo student was heading to middle school and loved soccer and swim practice, took dance and karate classes, and was a Girl Scout.
But in 2011, everything changed in a matter of weeks. Sara morphed from a sociable teen to a person who stopped talking and engaging with other people, and, at her worst, had full-blown catatonia.
Sara’s doctors were at a loss, but her mother, Eileen Quinn, wasn’t giving up. She embarked on what would become a 13-year quest, harnessing the power of a mother’s love to push the scientific community to pay attention to the mysterious regressions that some young people with Down syndrome were experiencing.
“I think people just might have a bias that, well, this person already has a disability, so it’s not as important,” Quinn said. “It was just devastating to think that I had lost Sara. I mean, this kid who made us laugh out loud every single day was totally gone. And there was just a shell left.”

A mystery illness was linked to Down syndrome. These moms found answers.
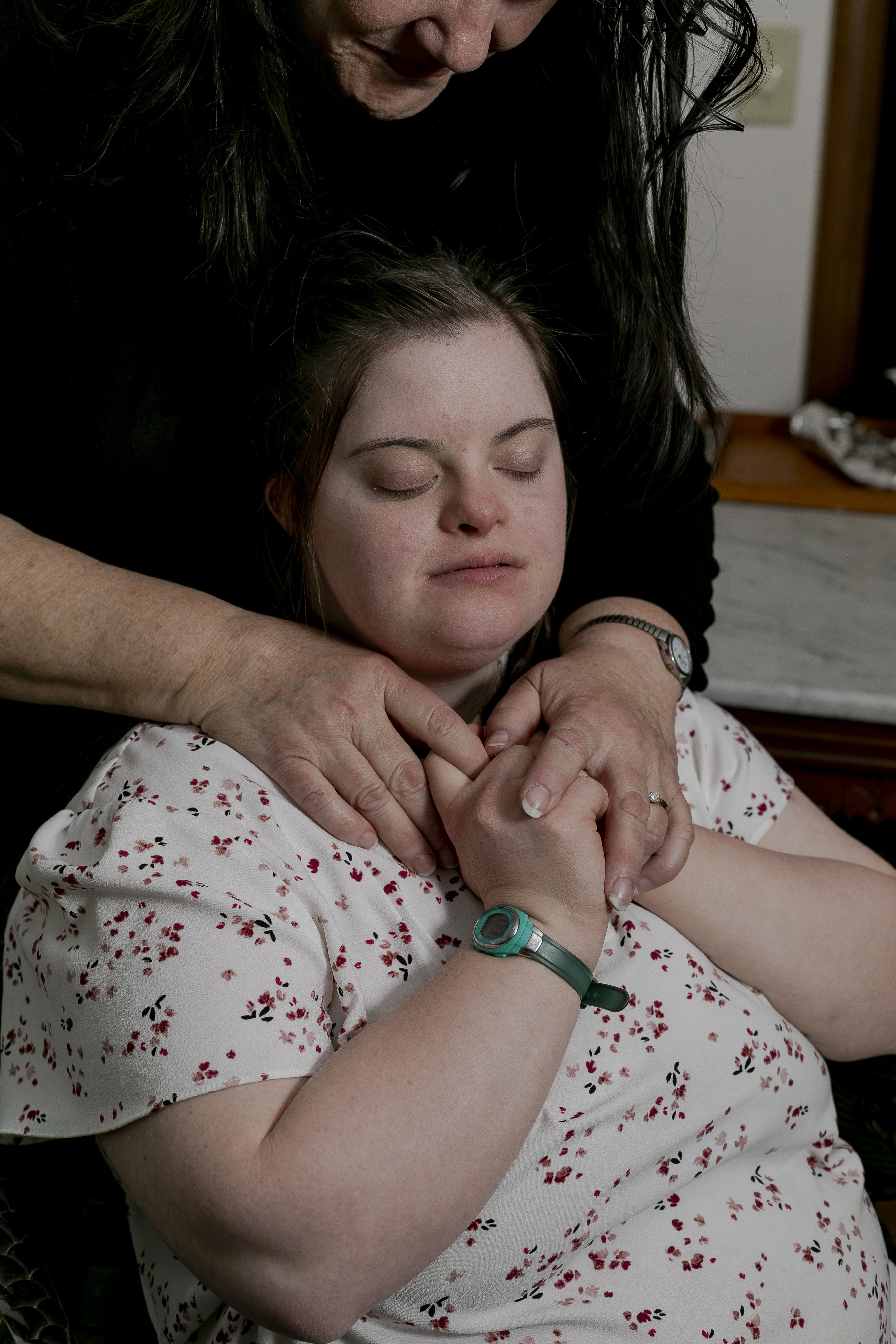
When Sara's doctors were at a loss to explain her condition, Quinn pushed the broader scientific community to pay attention.
As she searched for treatments for her daughter, Quinn, a developmental pediatrician at the University of Toledo, spoke at medical conferences and co-wrote research to spread the word. Through social media, Quinn galvanized other parents who also had seen their once-thriving children disappear. Quinn’s advocacy, combined with the efforts of another mother whose daughter had regressed, helped spur the first clinical trial of treatments for the regression disorder.
“She really gets a lot of credit shaking the consciousness of the community and saying, ‘There’s something new out there that we really need to target,’” said Brian Skotko, the director of the Down syndrome program at Massachusetts General Hospital and an associate professor at Harvard Medical School.

Sara, now 26, plays the board game Sorry with her 28-year-old sister, Bridget.
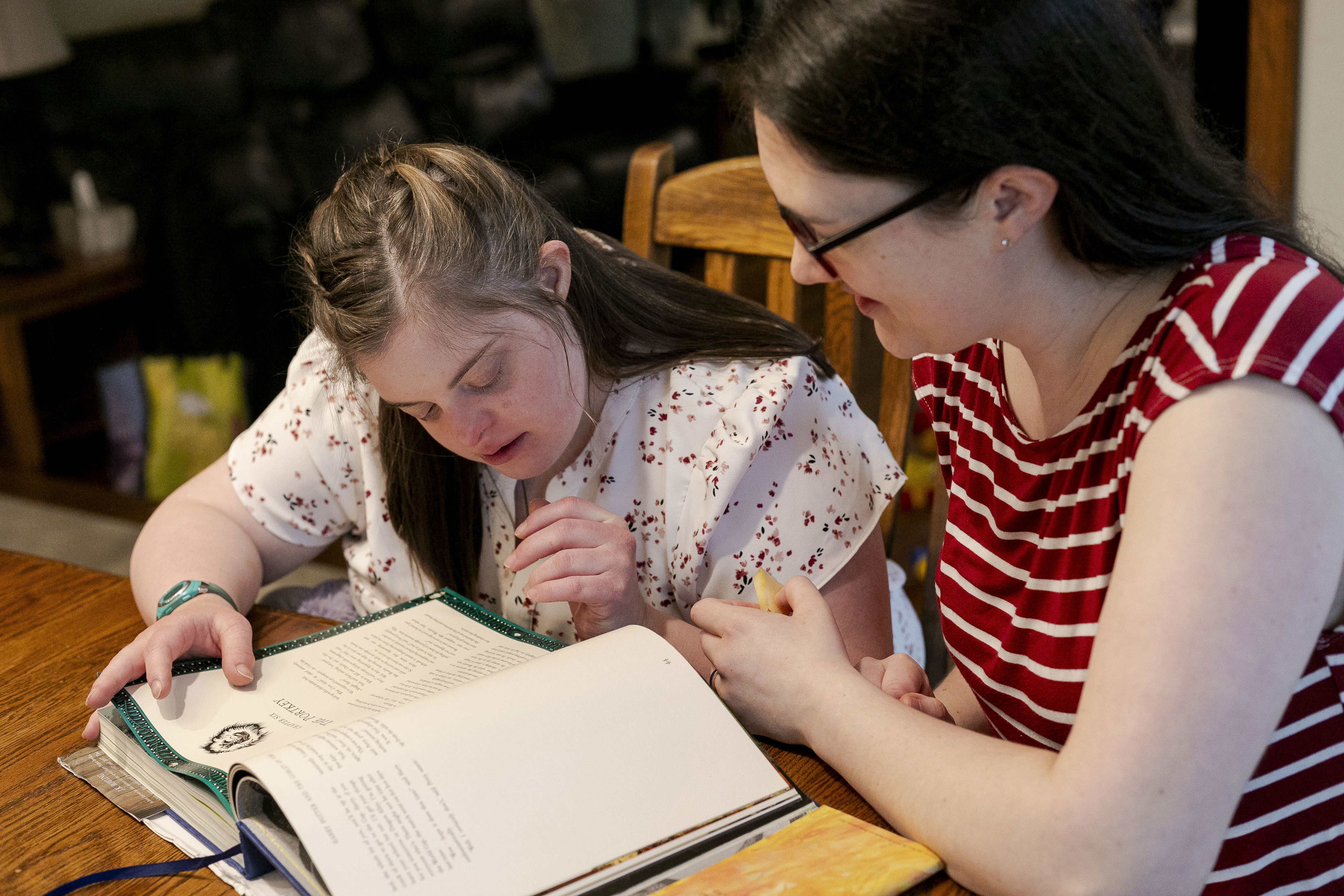
Sara reads a Harry Potter novel with her 32-year-old sister, Colleen.
A mystery condition that could hold clues to aging
Regression symptoms in patients with Down syndrome were identified as early as 1946, but the condition was often misdiagnosed as either early-onset Alzheimer’s disease or late-onset autism.
Its effects can be devastating. When someone with Down syndrome regresses, the decline can be precipitous and dramatic, with patients losing function in days or weeks, including the ability to talk, move or take care of themselves. Some, like Sara, can enter a catatonic state or suffer from hallucination and depersonalization, leaving loved ones desperately searching for answers and help.
For decades, there hadn’t been a formal diagnosis for patients experiencing regression symptoms. In fact, parents say doctors often would dismiss concerns, saying the regression was just a normal part of Down syndrome.
“I think people just might have a bias that, well, this person already has a disability, so it’s not as important.” Eileen Quinn, Sara Smythe's mother
It was only in 2022 that the condition was finally given an official name: Down syndrome regression disorder, or DSRD. Though its prevalence is difficult to measure, DSRD is believed to affect between 1 to 5 percent of people with Down syndrome.
Many believe a better understanding of Down syndrome, which occurs in approximately 1 in 800 births and is caused by an extra chromosome 21, could lead to advances in our overall understanding of cancer, autoimmune conditions and longevity. Remarkably, people with Down syndrome rarely develop hypertension as they age and almost never develop most solid tumor cancers. But they are far more likely to develop Alzheimer’s disease earlier in life. About 30 percent of people with Down syndrome develop dementia in their 50s.
Scientists who study Down syndrome say people with the condition live rich and fulfilling lives, but they also experience “a very atypical form of aging,” said Joaquin Espinosa, executive director of the Linda Crnic Institute for Down Syndrome at the University of Colorado Anschutz Medical Campus. For researchers, “that could be super-rich to understand aging in general.”

Miah Yager, now 31, developed Down syndrome regression disorder during her first semester at college, prompting her mother, Linda Roan, of Boulder, Colo., to launch a years-long search for treatment.
Galvanizing mothers
In 2013, before DSRD had been named or widely acknowledged by the medical community, Quinn joined a panel discussion of the Down Syndrome Medical Interest Group, which focused on the mysterious regression clinicians had been seeing in some patients with Down syndrome. Quinn presented her own daughter as a case study, including videos she had taken to document Sara’s decline. She noticed that their story brought tears to the eyes of some of those in the audience.
After the panel appearance, other families began to contact Quinn, desperate to talk with someone who understood the pain and isolation of watching a loved one regress. One of the first to reach out was Linda Roan of Boulder, Colo. Her daughter, Miah Yager, was 20 when she underwent a similar regression in 2013.
Gregarious and friendly, Miah had a natural talent for acting and had played a lead role as Lucy in the musical “You’re a Good Man, Charlie Brown.” Right after she graduated high school in 2012, Miah gave a speech at Purdue University as the youth keynote speaker for her church. The crowd gave her a standing ovation.
But in 2013, during her first semester at the College of Charleston, Miah began to disconnect from the outside world. Her friends noticed she was staying up for nights on end, obsessively copying notes and textbooks and missing appointments and social outings.
By Thanksgiving break, something was clearly amiss. The usually sociable Miah was not interested in being with her family and was suffering from the delusion that she was living in one of her favorite TV shows, “Pretty Little Liars.”
Miah didn’t return to school, and began what would become the first of many treatment attempts by her doctors. Over 18 months, psychotropic medications helped stabilize her, but it didn’t last. Miah regressed again and was no longer able to speak or answer questions. Roan had to feed her daughter by hand, rubbing her daughter’s cheeks to help her chew.
“I was like a bulldog trying to find some treatment and care for her,” Roan said.
Meanwhile, more and more families were reaching out to Quinn. In 2016, Quinn started a Facebook group called Regression in Down Syndrome. The private online community is now almost 2,000 strong, made up of family members — mostly mothers — seeking advice and trying to help their sons and daughters.
As more members joined the group, parents sought support, swapped tips and shared information about physicians and a variety of potential treatments, including psychotropic drugs and brain stimulation treatments. Some of the treatments helped for a while, but for many, including Miah, long-term success remained elusive.

Jonathan Santoro, an associate professor of neurology and pediatrics at the University of Southern California’s Keck School of Medicine in Los Angeles, spearheaded the 2022 paper defining DSRD.
‘It’s like they wake up’
In April 2020, at the start of the coronavirus pandemic, Jonathan Santoro, an associate professor of neurology and pediatrics at the University of Southern California’s Keck School of Medicine in Los Angeles, for the first time saw a patient with Down syndrome who had inexplicably regressed.
He ordered a lumbar puncture, which collects cerebrospinal fluid, and the test revealed proteins that suggested the patient’s blood-brain barrier had broken down, indicating the potential for inflammation in his brain. Santoro remembers running down the hallway to tell the patient’s father that he found something.
For Santoro, a trained immunologist and neurologist, it was an important clue. People with Down syndrome were already known to have a much higher rate of autoimmune disorders such as thyroid disorders, skin conditions and celiac disease. Santoro recalled thinking: “How is this not something autoimmune? This is exactly like so many of the other diseases I treat.”

Santoro opens a freezer holding biological samples from people with DSRD at his Los Angeles lab.
He and his team eventually treated that first patient with a standard immunotherapy called intravenous immunoglobulin, or IVIg, with a goal of resetting the immune system. After a combination of treatments, the patient dramatically improved. “Two weeks later, he’s running down the hall and hugging me and talking, and it’s like meeting a different person,” Santoro said.
“How is this not something autoimmune? This is exactly like so many of the other diseases I treat.” Jonathan Santoro, associate professor of neurology and pediatrics at the University of Southern California’s Keck School of Medicine in Los Angeles
When Santoro and his colleagues later followed 82 patients for up to a year after ending treatment with IVIg, they found that more than half remained well.
“When these treatments do work, it’s like they wake up,” Santoro said.
Santoro, who spearheaded the 2022 paper defining DSRD, said he believes that the regression symptoms had historically been downplayed by the medical community because of a bias many doctors may have about people with Down syndrome and intellectual disability.
“If you brought your perfectly healthy teenage son or daughter in and they were not sleeping, not eating, catatonic and hallucinating, we would admit them to the hospital and do a full workup,” Santoro said. “And we weren’t doing that with individuals with Down syndrome.”
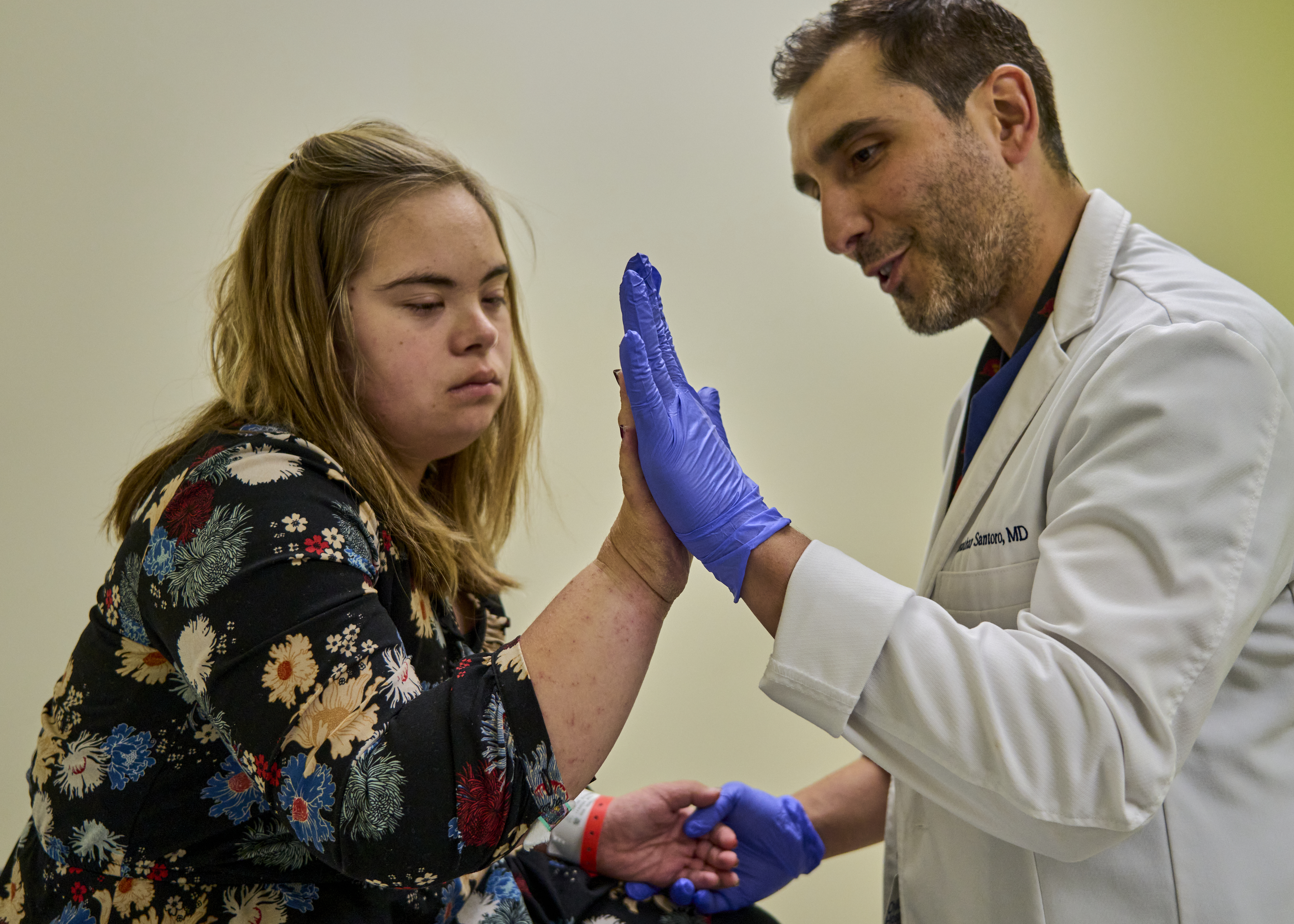
Santoro examines 17-year-old Brea Leavens, who has DSRD.
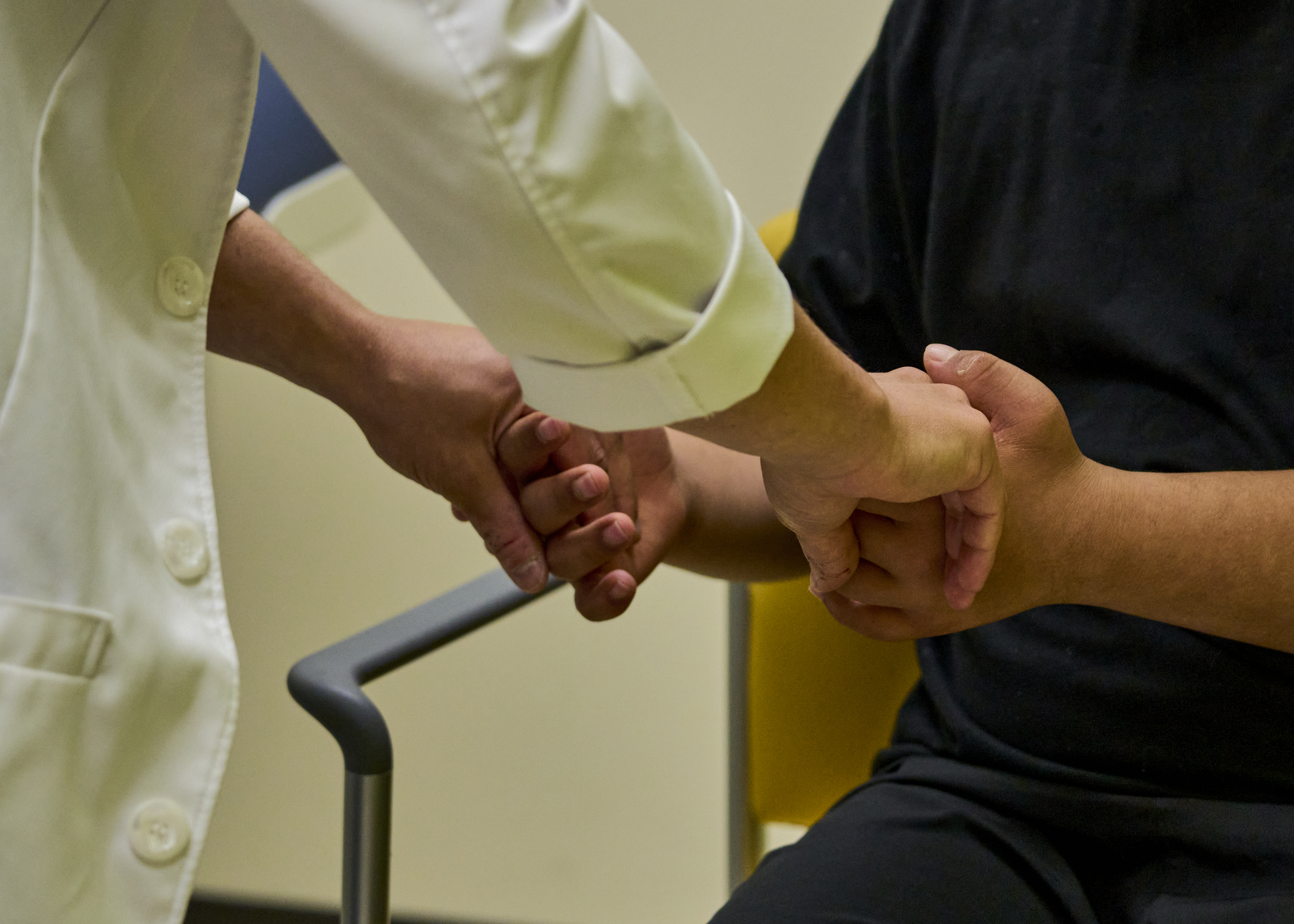
Santoro performs a neurological exam on 19-year-old Michael Reid, a DSRD patient.
A fortuitous connection
In October 2020, Santoro found Quinn’s Facebook group and asked to post about his research into the root causes of the strange regression disorder. Since then, hundreds of families have reached out.
Santoro and his team say they now have evaluated over 500 patients from all over the world, and many had abnormal brain scans or immune systems in overdrive, leading to inflammation that appeared to have affected their brains, possibly triggering the regression.
One of the patients Santoro treated was Miah. Unfortunately, the IVIg treatment he prescribed only helped a little, possibly because at that time, Miah already had been in regression for about seven years.
But the connection proved fortuitous in another way. After working with Santoro, Roan remembered meeting another researcher who had taken an interest in her daughter’s case and also told her he suspected the immune system may have played a role in her regression.
It was Espinosa, now executive director of the Linda Crnic Institute for Down Syndrome. He was researching immune system changes in Down syndrome as well as a more targeted form of immunotherapy.
Roan discovered that Espinosa and Santoro didn’t know of each other’s complementary research. She thought, “Oh, my gosh, these guys need to talk,” and introduced them over email.
“We hit it off right away,” Espinosa said. “So finally I found a partner who understands what we’re seeing.”

Researcher Joaquin Espinosa was investigating immune system changes in Down syndrome as well as a more targeted form of immunotherapy when Roan connected him with Santoro.
An immune system attacking the brain
In earlier studies, Espinosa and his colleagues had found that the stark uptick in immune activity in people with Down syndrome may lie on the extra copy of chromosome 21 that causes the condition. The chromosome contains important immune system genes for receptors that detect interferon, which allows our immune system to fight off viral infections.
But because people with Down syndrome have an extra chromosome 21, they have extra copies of these immune genes — which appear to dysregulate and ramp up the immune system’s response. The result, Espinosa said, is a body that acts like it’s “constantly trying to fight a virus that is not there.”
Now, researchers believe that people with DSRD may have a hyperactive immune system that’s mistakenly attacking the brain.
When Santoro and Espinosa began talking as a result of Roan’s introduction, they discovered they had both been working on different forms of immunotherapy treatments for Down syndrome patients. Santoro’s research focused on IVIg. Espinosa had been studying tofacitinib, an immunosuppressant drug that targets the interferon pathway and has been approved by the Food and Drug Administration to treat other autoimmune disorders, including rheumatoid arthritis, psoriatic arthritis and ulcerative colitis. Though Espinosa was testing tofacitinib for autoimmune skin conditions that afflict patients with Down syndrome, the treatment had also shown promise in patients with DSRD, including Miah.

Espinosa, executive director of the Linda Crnic Institute for Down Syndrome at the University of Colorado Anschutz Medical Campus, with Kelly Sullivan.
To compare the treatments side by side, the researchers designed a trial pitting lorazepam, a standard psychiatric drug, against each of the two immunotherapies. In 2023, Santoro and Espinosa, along with Elise Sannar, a child psychiatrist at Children’s Hospital Colorado, established the first randomized control clinical trial of potential treatments for DSRD.
The researchers are working together to collect as many biological specimens as possible to understand both what causes DSRD as well as what biological signatures could help predict the most effective treatment for each patient.
Espinosa credits Miah and Roan for this collaboration. “It was really the story of this participant and this mom that brought us all together,” he said.
Roan now works with Espinosa at the Crnic Institute as the clinical trial community liaison, a role in which she draws on her experience as a parent and caregiver to explain the research and treatments to other families.
“My hope is — and I believe this to be true — that no families are going to have to go through what my family, what Miah’s been through,” Roan said.
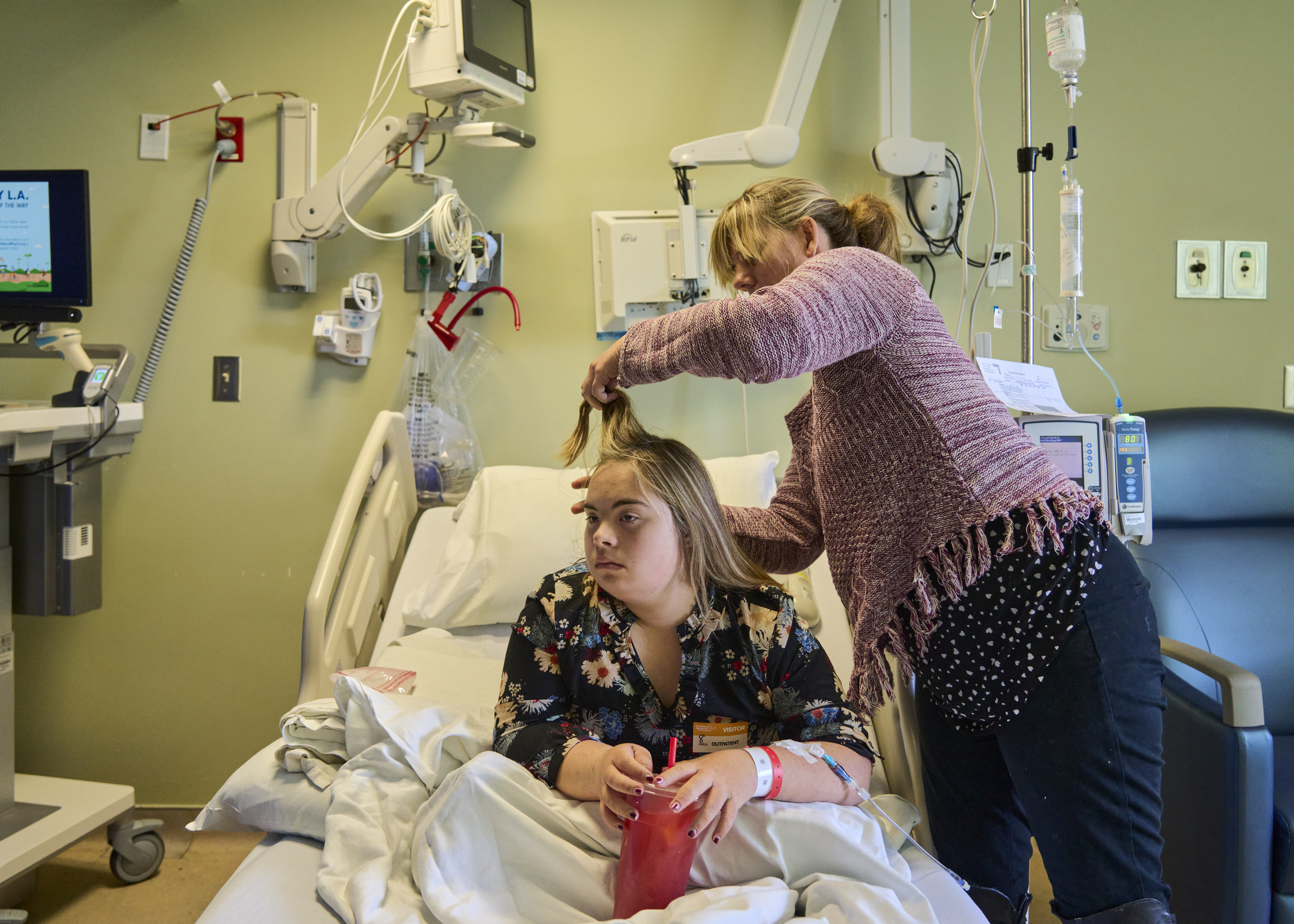
Brea receives an infusion to treat DSRD at Children's Hospital Los Angeles.

Michael puts his arm around his mother at Children's Hospital Los Angeles.
Spreading the word about DSRD
Santoro and Espinosa want to create more awareness of DSRD so doctors and patients can seek treatment sooner. They’ve conducted workshops with the Global Down Syndrome Foundation and the National Down Syndrome Society. To help, Quinn continues to offer resources through the Facebook group and has held webinars and podcasts with Santoro to help spread the word.
The rapid progress in research and awareness about DSRD reached the small town of Eagle River, Alaska. That’s where 27-year-old Darci Owens was living when she began to regress.
Owens, who has Down syndrome, was the first athlete in Alaska to become a certified coach through Special Olympics and traveled with the Seattle Seahawks for fundraising events. She hosted a cooking show on Facebook called “Dining With Darci,” teaching Special Olympics athletes how to make healthy meals and snacks, including fish tacos made from Alaska halibut, her favorite recipe on the show.
But on April 11, 2022, Darci’s life changed. That week, she became mute and would not eat. She could no longer run without falling, and quickly developed psychosis, which meant the once-independent athlete had to be fed, bathed and dressed.
Her mother, Dana Owens, a manager of therapy services at a hospital, found Quinn’s Facebook group as well as Santoro’s research on DSRD. Dana got in touch with Santoro and flew to Los Angeles with Darci for testing. Santoro recommended IVIg and provided Darci’s doctors in Alaska with detailed protocols for treatment.
With a combination of IVIg, electroconvulsive therapy and lorazepam, Darci, now 28, emerged from the depths of regression and catatonia. Most, but not all, of her symptoms have now abated, and she is continuing to undergo treatments. “But overall, oh, such vast improvement from where we were,” Dana Owens said.
The road ahead for Miah
Miah, now 31, started on tofacitinib in 2021 as part of Espinosa’s clinical trial on autoimmune skin conditions. Though the tofacitinib only partially helped her skin condition, Miah’s regression symptoms improved.

Miah, playing Sally Brown in “You’re a Good Man, Charlie Brown,” strikes a pose during a dress rehearsal in November.
In November 2023, Miah was focused on rehearsing for a musical, “You’re a Good Man, Charlie Brown” — the same one she had starred in 12 years prior. “I’ve been practicing my play a ton, so that’s fun,” Miah said over a plate of chicken tacos at the taqueria next door to the dress rehearsal, where she danced and sang in her role as Sally, the titular character’s younger sister.
But DSRD has taken its toll.
“Her memory is pretty much wiped out, like, she has no memory — not even just of DSRD, but even the good times back to high school,” Roan said. Miah does not remember that she had performed in this musical before as its star.
Miah still experiences flare-ups and periods of relapse in which she feels “fuzzy” and “heat” in her head, as she describes it. Last fall, Miah said she still felt a “medium heat” but she continues to improve. She is training to be a waitress, a job in which she enjoys getting “to meet new people every day,” and lives five nights a week with two roommates who give her extra support.
“She’s never gotten fully 100 percent back to the person that she was prior, but she’s pretty darn close, and she’s doing well,” Roan said.
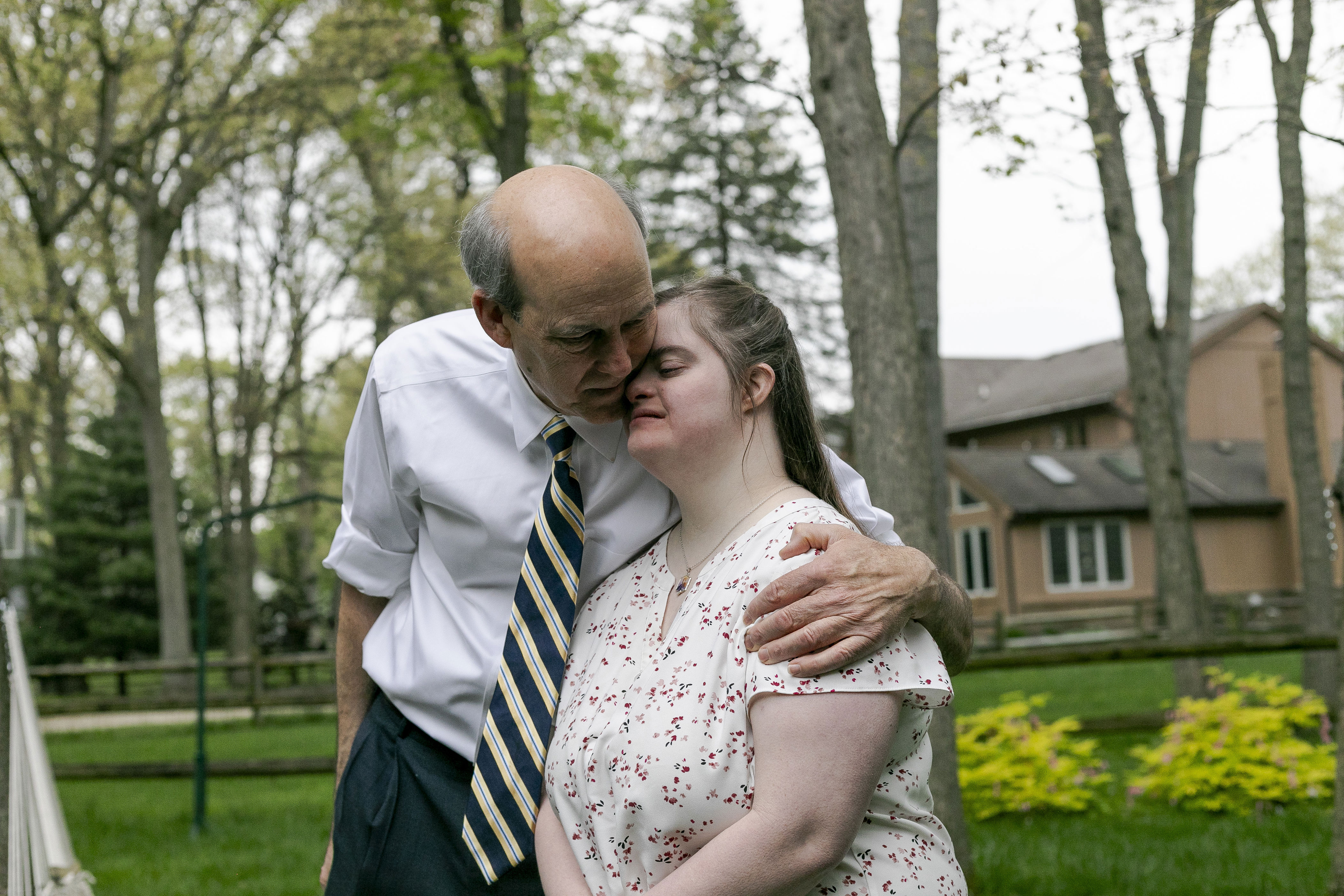
Pathologist Peter Smythe, Sara's father, holds his daughter in their backyard in Toledo.

From left, sisters Bridget, Sara and Colleen Smythe lie in a hammock in their family's backyard.
A formal diagnosis for Sara
In June 2023, Quinn and Sara flew to see Santoro, who officially diagnosed Sara with DSRD. Sara received her first dose of IVIg in mid-October that year. Like Miah, Sara hasn’t returned to who she was before regression, but she is improving.
Recently, Sara was part of a performance for an ice-skating program called Gliding Stars. Sara smiled during the performance, which she hadn’t done in the 10 years she had previously participated, Quinn said. Sara, now 26, recently graduated with a certificate from the University of Toledo transition program for people with disabilities. She has also become more social and recently attended the wedding of a friend from grade school.
While the improvements aren’t dramatic, they are significant. The immunotherapy has given Sara back “joy and the capacity to show it,” Quinn said.
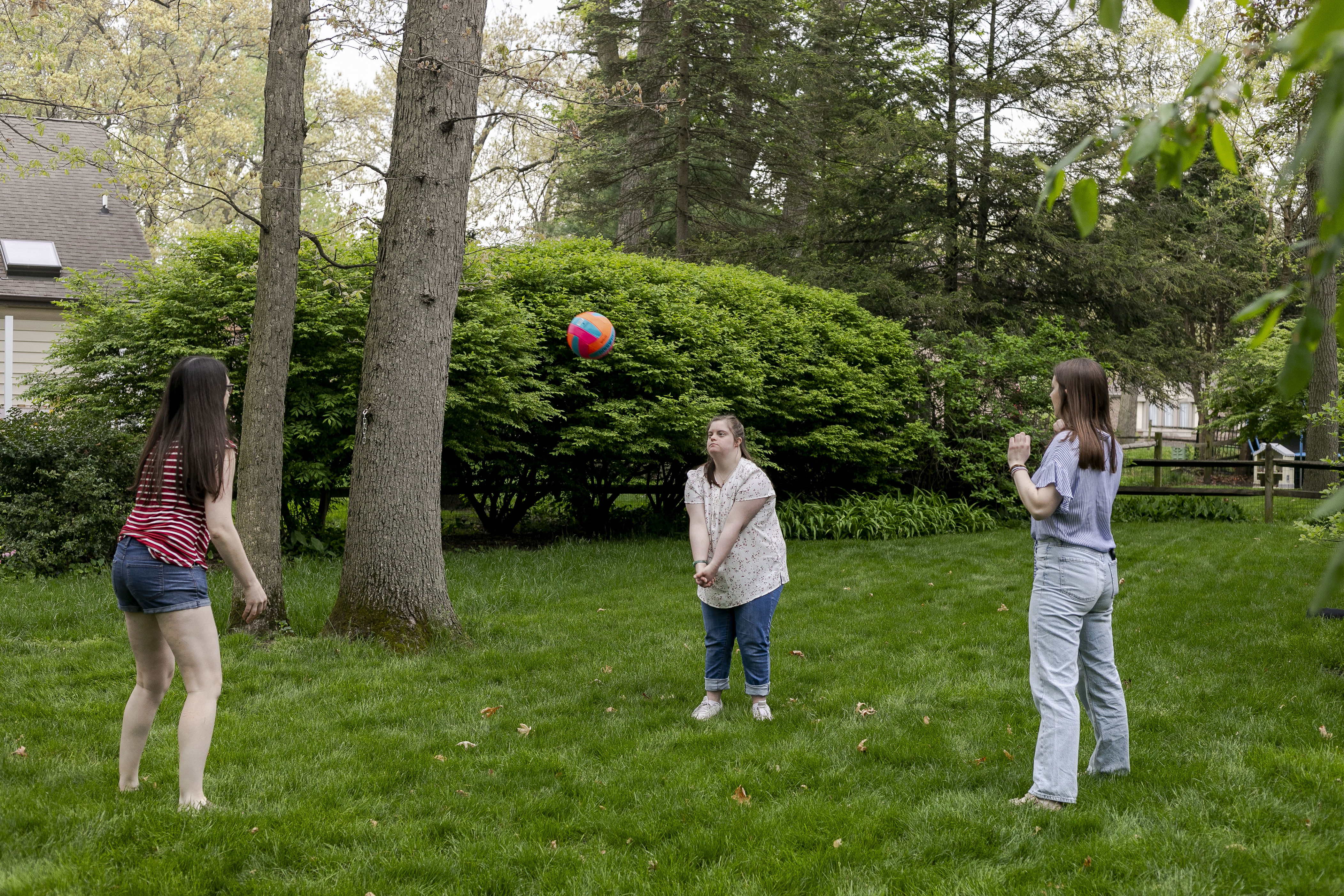
The Smythe sisters play volleyball in the backyard. Since Sara began immunotherapy, her condition has shown signs of improving, Quinn said, and she has regained “joy and the capacity to show it.”
